This article promotes a
Better
understanding of atherosclerosis--the inflammation and buildup
of fatty deposits in blood vessels--has triggered new approaches
to
treating the nation's leading causes of death
by Delia K. Cabe
Blood vessels are built to last. Up to about 100 years, some experts say, under normal wear
and tear. For that to happen, you not only have to abide by a heart-healthy lifestyle--low-fat diet, weight in check, exercise,
stress management, blood pressure control, good cholesterol numbers, moderate alcohol use, no smoking--but you also should
be a woman, have the right genes and age slowly.
Cut to reality: we're not perfect. Our blood vessels endure various assaults because of factors
only some of which we can control. We get heart disease--some 14 million Americans have it, and 500,000 die from heart attacks
annually. The older we get, the more likely it is we'll end up with it. The proof is in the numbers: heart disease affects
an estimated 15 percent of adults in their late 30s to early 40s, about 50 percent of 55- to 64-year-olds, and 65 percent
of those in the next decade. Obviously, many of us slept through Heart Disease Prevention 101.
Yet the heart cognoscenti say only half to three fourths of heart disease cases result from
the established risk factors. The rest come about from infection and other factors that may promote atherosclerosis, the buildup
of fatty deposits in blood vessels. Indeed, current research indicates that all of us are in jeopardy from the leading cause
of death in the U.S. Everyone needs to maintain a healthy lifestyle, says endocrinologist Joanne Manson, chief of the division of preventive medicine at Brigham and Women's Hospital in Boston. Everyone's
at risk.
Efforts to Þnd additional means of preventing heart disease have led to the unearthing of about
300 predictors, including bad relatives of the troublemaker cholesterol as well as bacteria and baldness. Yes, baldness.
Manson and her colleagues at Harvard Medical School, which is afÞliated with Brigham and Women's
Hospital, published a study this year that found that hair loss, speciÞcally on the crown of the head rather than at the front,
is linked to a threefold greater risk of heart disease in men. Blame it on male hormones. The connection may be elevated androgen
levels, which are associated with baldness and have been linked to atherosclerosis and a higher risk of blood clotting.
Such a marker as baldness may seem an unlikely place to look for risk factors. But in 1988 Manson's
group also found a correlation between height and heart disease. Let's just say that taller people are better off--perhaps
because they have wider blood vessels. Such information may help identify people who are more prone to heart disease and may
lead to better means for prevention and interruption of disease progression tailored to an individual's physiology. The discovery
of many of these markers arose from a closer examination of the cycle of inþammation, plaque formation and injury that causes
atherosclerosis, the forerunner to angina and to heart attack and stroke, the major causes of death and disability as we move
into later life.
The broadened understanding of the underlying causes of heart disease has paved the way to potential
therapies, including antibiotics and ACE (angiotensin converting enzyme) inhibitors. ACE inhibitors were developed to control
high blood pressure, but they have recently been found to have therapeutic effects in preventing heart disease.
Read My Lipids
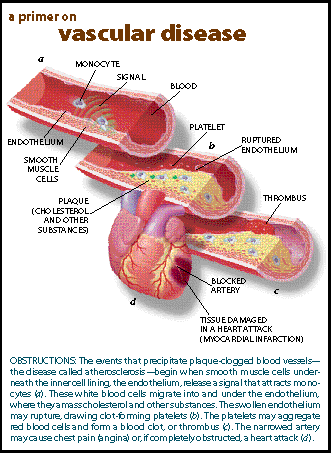
Atherosclerosis, which begins in our teenage years and builds up as we age, starts when the smooth muscle cells
underneath the endothelium, or inner lining, of blood vessels release a signal in response to high cholesterol levels. This
signal attracts monocytes--white blood cells that Þght infection and amass cholesterol, calcium and other substances. The
resulting cheesy mass, or plaque, bulges like a pimple. Over time, the endothelium loses its elasticity and may rupture.
|
Illustration: Dusan Petricic |
This injury to the lining summons clot-forming platelets, which further restrict blood þow through
the already narrowed artery. An inadequate supply of oxygen-rich blood to heart muscle may cause temporary chest pain, or
angina, and if blood þow is completely cut off, a heart attack--in clinical terminology, a myocardial infarction. All this from the best-known harbinger of heart trouble, the lipid cholesterol. But only to a
degree.
Cholesterol has been the cause célèbre in heart disease prevention. Fifty percent of Americans
have elevated cholesterol levels. And the increase occurs naturally as we age--mostly after about age 45 for men and age 55
for women. Women in their reproductive years tend to have lower levels than men of the same age. After menopause, their cholesterol
levels rise. But we also should fault our lifestyles. Without a doubt, lowering dietary intake of cholesterol and saturated
fats does wonders for the heart. The goal is to keep down blood levels of the bad cholesterol (low-density lipoprotein, or
LDL), behavior that can produce a 25 to 35 percent reduction in what the pros term "cardiovascular events"--that is, heart
attacks, strokes and the like. At the same time, don't forget about raising your levels of good cholesterol (high-density
lipoprotein, or HDL), which mops up LDL.
But the picture's more complex. Some people develop heart disease in spite of attaining ideal
lipoprotein levels. For them, an approach that goes beyond controlling cholesterol and other lipids may be in their future.
Six years ago researchers with the Framingham Heart Study (the decades-long study that brought us the term "risk factor") identified a relative of LDL called
lipoprotein(a) as an independent risk factor for heart disease. Lp(a) fosters the deposition of cholesterol on artery walls
and interferes with the body's means of dissolving clots. Lp(a) also enhances oxidation of LDL.
Oxidation is nature's way of spoiling things like food. But old food gets thrown out, whereas
oxidized LDL stays in the bloodstream and penetrates the endothelium. Elevated levels of Lp(a), which are most likely genetic,
place people in the "high risk" category, as would a total cholesterol level greater than 240 milligrams per deciliter of
blood (mg/dl) or an HDL level less than 35 mg/dl. Blood tests to measure Lp(a) have become available, but Lp(a) is difÞcult
to lower. Two therapies that show promise include the vitamin niacin at prescription doses that are 100 times higher than
the recommended daily allowance and the hormone estrogen. In addition, a few studies suggest that reduction in LDLs may help.
But it now seems that some LDL particles are worse than others. In the few studies done to date,
people with predominantly small LDL particles have a risk of heart disease between three and four and a half times greater
than those with large LDL particles. Why does size matter? Small particles are more prone to oxidizing, damaging blood vessel
walls and invading them 50 percent faster than larger particles to initiate cholesterol accumulation.
Looking for Little Stuff
Ablood test to measure LDL particles is useful in determining which drugs would be most effective
in individuals with heart disease or in those who have a strong family history of it. Fortunately, current heart disease interventions
cut down small-particle LDL levels. These include exercising, taking niacin (but only under a doctor's supervision) or some cholesterol-lowering drugs. Diet can also help
lower triglycerides (another type of fat in the blood).
|
Illustration:
John W. Karapelou
|
Even the good cholesterol, HDL, turns into a traitor in certain environments, much like a chameleon
changes its colors in different surroundings, says cardiologist Alan M. Fogelman, executive chairman of the department of medicine at the University of California at Los Angeles
School of Medicine.
Normally, HDL prevents LDL oxidation. But he and other researchers have observed HDL in its
other guise. After surgery or during infections, atherosclerotic plaques burst more easily. These ruptures may occur because
the immune system has geared up to Þght infection. In this environment, HDL changes into a molecule that promotes LDL oxidation.
If studies bear out this model, researchers could develop medications to thwart HDL's metamorphosis.
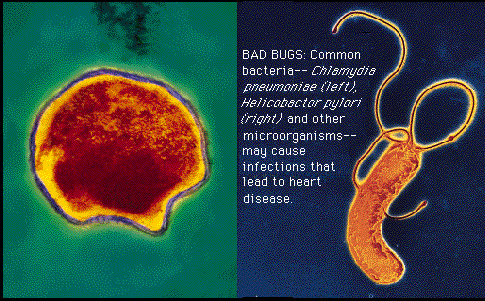
The possibility that the inþammation within the blood vessel walls and the immune system's response
might be triggered by an infection led investigators to two bacteria--Chlamydia pneumoniae and Helicobacter pylori (the latter was recently deemed the culprit in stomach ulcers)--and herpesvirus. Of these three,
C. pneumoniae, which causes respiratory infections, has received the most attention. The burning question is whether this
bacterium, which has been found in 70 to 80 percent of plaques taken from heart disease patients, is an innocent bystander
or an accomplice.
Cardiologists Jeffrey L. Anderson and J. Brent Muhlestein of the University of Utah are among several researchers looking for the answer. But these two
colleagues were not about to take their cue from the scientist who gave himself an ulcer by ingesting H. pylori. Instead of
hardening their arteries in the name of medicine, Anderson and Muhlestein opted for studies on other animals. They set about
infecting rabbits, which normally do not develop atherosclerosis, with C. pneumoniae. Plaques did indeed appear, and antibiotics
reduced the number of these thickenings.
Having shown cause and effect, the researchers set their sights on humans with heart disease
who had evidence of past infection with C. pneumoniae. After six months on the antibiotic azithromycin, the human subjects
had a modest but signiÞcant reduction in key markers of blood vessel inflammation: C-reactive protein, tumor necrosis factor,
and the interleukins IL-1 and IL-6, all of which are released by the immune system. At the end of two years, Anderson and
his colleagues hope to see at least a 50 percent reduction among those treated with the antibiotic in the frequency of heart
attacks, angina, stroke, and procedures such as angioplasty and bypass surgery.
Anderson is among the investigators taking part in long-term trials now under way at several
medical institutions with large numbers of human subjects. If antibiotics do signiÞcantly reduce the incidence, physicians
say this would be a major advance in heart disease treatment. Heart patients who show these inþammatory markers might be prescribed
medication to combat the bacteria. Until that time, though, I think we shouldn't be giving antibiotics to our patients, Anderson
says, because studies are still ongoing.
Meanwhile cardiologists are assessing whether taking folate and other B vitamins might lower
heart disease rates. Accumulating evidence from the Physicians Health Study, the Framingham Heart Study and others seems to
point to a direct relationship. And homocysteine levels in blood could be the smoking gun. Homocysteine, an amino acid that
results from the body's metabolism of food, may contribute to atherosclerosis and increase clotting because it makes platelets
stickier. In addition, homocysteine may lessen the þexibility of blood vessels, slowing blood þow. In people such as older
adults and postmenopausal women, who typically have high levels of homocysteine in their blood, the risk of heart attack and
stroke increases. Folate and other B vitamins may bring about a decrease in heart disease risk because they break down homocysteine.
Folate in Your Diet
Randomized, controlled trials are needed to determine if managing homocysteine levels, as is
done with cholesterol, could join the list of heart safeguards. Nevertheless, the American Heart Association currently advocates that people who are at high risk for heart disease include more folate and
other B vitamins in their diet--at least 400 micrograms' worth. That deed is accomplished simply by eating a balanced diet
that includes the already recommended Þve daily servings of fruits and vegetables.
High blood pressure, or hypertension, was long ago shown to predispose people to atherosclerosis,
heart attack and stroke. Hypertension is indeed an affliction of aging. The number of men and women with high blood pressure
rapidly escalates in older age groups. More than 50 percent of Americans over age 65 have high blood pressure. First-line
treatment to control hypertension involves a healthy diet, exercise and weight loss. If that fails, physicians prescribe antihypertensives
such as ACE inhibitors. Until the 1980s, the presumed and only beneÞt of ACE inhibitors was the foiling of the body's production
of angiotensin, a chemical that constricts arteries, so that blood can þow through vessels easier. But new research indicates
that ACE inhibitors do more. So much more that the HOPE study evaluating the effects of the ACE inhibitor ramipril in 9,541
heart disease patients at multiple medical institutions was stopped six months early and its results released last November,
before publication, so that study participants receiving a placebo could also reap the drug's beneÞts.
We got stunning results--more than we expected, says study chairman and cardiologist Salim Yusuf of McMaster University in Ontario. "It is like the discovery that cholesterol drugs lower risks
of heart attacks." The data showed a 22 percent overall reduction of heart attacks, stroke or death from other cardiovascular
causes. The beneÞt was independent of ramipril's small reduction in blood pressure. In fact, most of the participants did
not have hypertension when they enrolled in the study. Ramipril, Yusuf adds, may have an important effect within blood vessel
walls, but it is unknown if other ACE inhibitors work in a similar fashion. Now physicians can offer one more preventive approach
to their patients.
But these pills and other advances are meant for those of us who
have flaunted time-tested heart-saving advice or the few who have only their genes to blame for abnormal lipid levels and
such. As for waiting for that quick Þx, researchers promise none. You can hope and pray. Take it from the grand pooh-bah of
heart health, American Heart Association president Lynn A. Smaha: New research Þndings hold promise but no certainty of licking
heart disease, so in the meantime, take care of yourself.